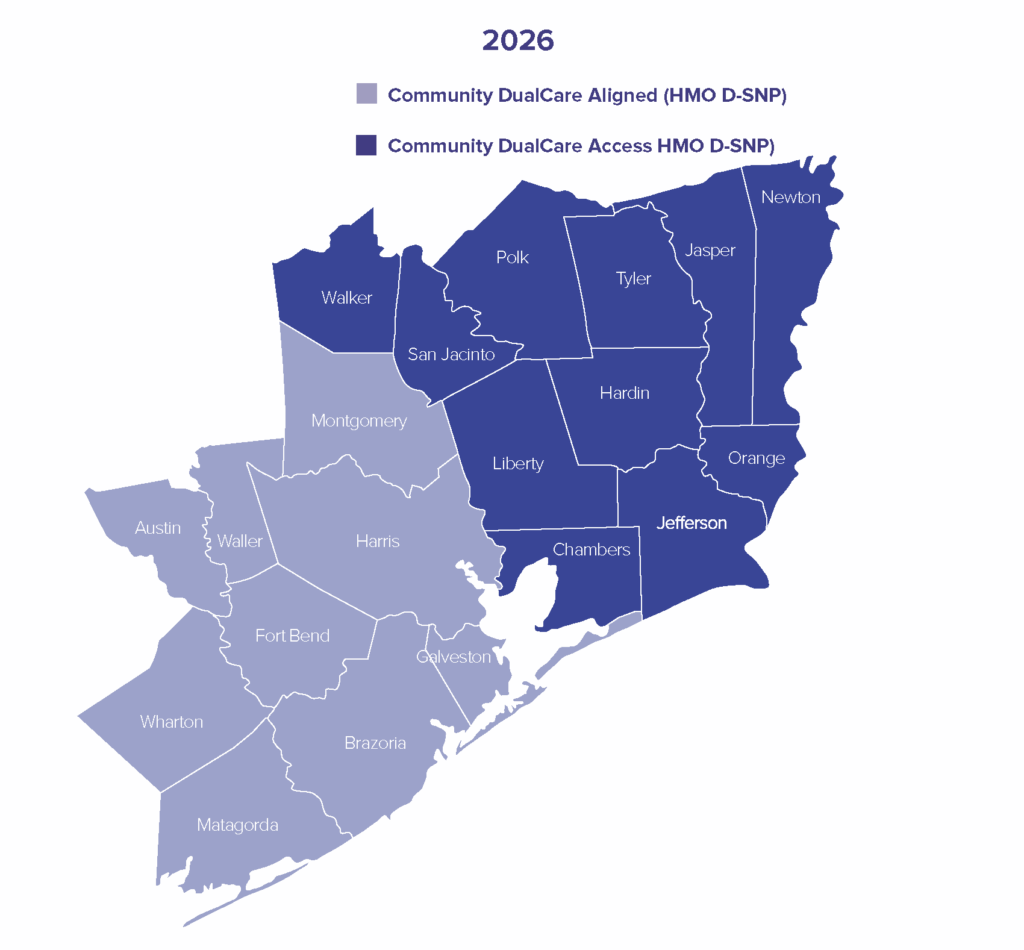
The Texas counties in the service areas covered by Community DualCare Access (HMO D-SNP) in 2026
Chambers, Hardin, Jasper, Jefferson, Liberty, Newton, Orange, Polk, San Jacinto, Tyler, and Walker.
The Texas counties in the service areas covered by Community DualCare Aligned (HMO D-SNP) in 2026
Austin, Brazoria, Fort Bend, Galveston, Harris, Matagorda, Montgomery, Waller, and Wharton.